Chronic Venous Insufficiency (CVI)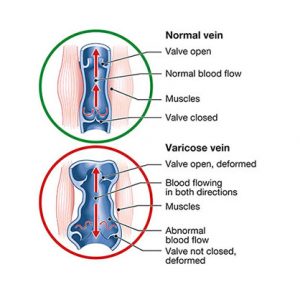
Chronic venous insufficiency occurs when your leg veins do not allow blood to flow back up to your heart. Normally, the valves in your veins make sure that blood flows toward your heart. But when these valves do not work well, blood can also flow backwards. This can cause blood to collect (pool) in your legs.
Chronic venous insufficiency is not a serious health threat. But it can be painful and disabling.
What causes chronic venous insufficiency? Learn More Close
The causes of chronic venous insufficiency include:
- High blood pressure in the leg veins over time, due to sitting or standing for long periods
- Lack of exercise
- Smoking
- A blood clot in a deep vein, often in the calf or thigh (deep vein thrombosis)
- Swelling and inflammation of a vein close to the skin, often in the legs (phlebitis)
Who is at risk for chronic venous insufficiency? Learn More Close
You are more at risk for this condition if you:
- Are overweight
- Are pregnant
- Have a family history of it
- Have had damage to your leg because of injury, surgery, or previous blood clots
What are the symptoms of chronic venous insufficiency? Learn More Close
Symptoms of chronic venous insufficiency may include:
- Swelling in your legs or ankles
- Tight feeling in your calves or itchy, painful legs
- Pain when walking that stops when you rest
- Brown-colored skin, often near the ankles
- Varicose veins
- Open sores on the legs (leg ulcers) that are sometimes hard to treat
- An uncomfortable feeling in your legs and an urge to move your legs (restless legs syndrome)
- Painful leg cramps or muscle spasms (charley horse)
These symptoms may seem like other health problems. Talk with your healthcare provider for a diagnosis.
How is chronic venous insufficiency diagnosed? Learn More Close
Your healthcare provider will take your health history and give you an exam. You may also have an imaging test called a Venous Duplex ultrasound. This looks at blood flow and the structure of your leg veins. It checks the speed and direction of blood flow in the blood vessel.
How is chronic venous insufficiency treated? Learn More Close
Treatment will depend on your symptoms, age, and general health. It will also depend on how severe the condition is.
Treatment may include the following.
Doing things to improve blood flow in your leg veins
Keeping your legs raised (elevated), wearing compression stockings, good skin care, healthy body weight, and exercising regularly may help.
Taking medicines
Medicines that increase blood flow through the vessels may be used along with compression therapy to help heal leg ulcers. Aspirin can also be used to help ulcers heal. Medicines that draw excess fluid from the body through the kidneys (diuretics) are not often used. But they may be taken if other conditions such as heart failure or kidney disease are also linked to the swelling.
Having sclerotherapy
This may be used if you have spider veins or small varicose veins. A chemical is injected into the affected veins. The chemical causes scarring in the veins so that they can no longer carry blood. Blood then returns to the heart through other veins. The body absorbs the scarred veins.
Having endovenous laser ablation or radiofrequency ablation (RFA)
This is a minimally invasive procedure. A tube (catheter) puts heat right into the affected vein. This closes the vein. Once the vein is closed, less blood pools in the leg. Overall blood flow is improved.
Having surgery
This is done in severe cases. Ligation is a type of surgery that may be used. The affected vein is tied off so that blood no longer flows through it. If the vein or its valves are heavily damaged, the vein will be removed. This is called vein stripping.
Key points about chronic venous insufficiency Learn More Close
- Chronic venous insufficiency occurs when your leg veins do not allow blood to flow back up to your heart.
- Symptoms include pain, swelling, cramps, and skin changes.
- Some common causes are being overweight and having damage to a leg, such as from an injury.
- An imaging test called a Venous duplex ultrasound can diagnose it.
- Compression socks and medicines may work for milder cases. More serious cases may require sclerotherapy or surgery.

